I have always had a healthy appetite, so watching my daughter subsist on two blueberries was baffling and concerning. Despite eating ‘solids’ for over 18 months, I could only recall her requesting food a handful of times.
But today something rare happened.
Sienna uttered the words “num num” (translation: “I want food“).
When offering her a bite of anything edible, 99.95% of the time her response is “No num num” (translation: “I don’t want food“), so I asked her to clarify. Turns out it wasn’t my imagination…
Sienna was indeed asking for something to eat. These words were music to my ears.
In fairness to my daughter, she doesn’t experience feelings of hunger like the average person. From what we know thus far, her appetite is significantly diminished as a result of her RSS diagnosis. While my little one has a medical condition limiting her desire to eat, children like her aren’t the only ones with a dampened appetite.
UPDATE AS OF AUG 2018:
Sienna is now 5 years old and her appetite is going strong. This child is always hungry, loves all varieties of food, and she’s costing me a fortune. But I am not complaining! Every time I read this post from a few years ago I’m reminded of our former struggles at the table. And I’m so grateful I made these changes then.
Had we continued down the same path of giving Sienna her favourite foods, sneaking veggies, and bribing her with TV/toys/cookies, we would not be where we are today…
Enjoying mealtimes with a little girl who loves to eat. Even mixed textures like this fish stew (wha!).

Are you wondering why your little one never seems hungry?
Let’s look at a few ways to increase a child’s appetite.
While a more in-depth nutritional assessment helps parents identify underlying reasons for poor eating, let’s start with a few tips to improve appetite.
1) Avoid all-day grazing
You would think that letting our children snack all day would result in them eating MORE food. Right?
Researchers tell us the opposite is true.
If your little one is given a bite of food throughout the day, he/she won’t have the opportunity to truly experience hunger. So his or her appetite may simply be a result of the current feeding structure (or lack thereof).
Toddlers should have a 2-3 hour gap between each meal or snack, and 3-4 hours for older children.
That means no nibbles, no milk, no juice, not even one itsy bitsy Gold Fish.
Nada.
Just offer water.
To save you from temper tantrums, I recommend making the transition slowly if your child is used to grazing. Start by stretching the non-eating window by 15 minutes every few days, or if your little one is old enough, simply explain that “we are making some changes to how often we eat, so you can spend more time playing”.
You’d be surprised how an appetite miraculously appears when we remove the all day nibble sessions.
2) Keep an eye on iron
Iron is a buzz-word these days when it comes to children’s nutrition; your pediatrician is likely encouraging you to feed your little one meats as a first food when introducing solids.
Why this iron push?
Well, an infant’s iron stores decline around 6 months of age and studies show that at least one in eight toddlers is anemic before they are 2 years old.
While iron deficiency tends to diminish appetite, the risks for our kiddos does not stop there. Iron deficiency in the first years of life has also been linked back to cognitive, motor, and behavioral deficits (Lozoff et al. 2006). So lots of good reasons to keep an eye on iron.
 How much does your child need daily?
How much does your child need daily?
- 6-12 months: 11 mg
- 1-3 years: 7 mg
- 4-8 years: 10 mg
- 9-13 years: 8 mg
Iron boosters:
- Pair Vitamin C foods with iron sources to improve absorption.
- Cook foods in a cast iron pan. You’ll get best results by cooking moist, acidic foods like applesauce, chili, tomato sauce, stew, and scrambled eggs.
- Limit foods rich in phytates which can reduce iron absorption by up to 80% (includes plant-based foods such as nuts, seeds, grains, and some vegetables). Phytates or phytic acid can bind to zinc, iron, and other minerals decreasing their absorption. Here are two tips: (1) soak nuts, legumes, etc. to reduce the amount of phytates consumed with these foods or (2) pair vitamin C with these foods to help counteract the effect. (Source)
- Avoid dairy products (calcium inhibits absorption of iron), particularly when iron and calcium food sources are being eaten at the same time.
- Introduce more sources of iron in your child’s diet. See below.
Iron Sources: (extensive list here)
- Ground beef (2.5 oz) — 1.3-2.2 mg
- Chicken liver (2.5 oz) — 6.2-9.7 mg
- Lentils (1/2 cup, canned) — 3.2 mg
- Eggs (1 egg yolk) — 0.46 mg
- Cooked Spinach (1/4 cup) — 1.6 mg
- Fortified oatmeal (5 Tbsp) — 3.66 mg
3) Keep an eye on zinc
Zinc is an essential mineral required for many physiological functions, including immunity (i.e. fewer colds and illnesses), antioxidant function, growth and reproduction.
A mild deficiency can lead to poor appetite, weight loss, diarrhea and increased susceptibility to infections. As a zinc deficiency progresses it can lead to growth failure, delayed healing of wounds, short stature, and hair loss. Acute depletion of this mineral can cause an altered sense of taste and smell, and given that zinc stores decrease with age, we can understand why elderly people experience a loss in appetite.
 How much does your child need daily?
How much does your child need daily?
- 7-12 months: 3 mg
- 1-3 years: 3 mg
- 4-8 years: 5 mg
- 9-13 years: 8 mg
Zinc boosters:
- Vitamin D improves absorption of calcium, magnesium…and zinc! So why not add your child’s vitamin D drops to their scrambled eggs, oats, or any other food high in zinc.
- Spread your zinc intake throughout the day versus higher doses in one meal. One study shows that consuming larger amounts of zinc results in a smaller percentage being absorbed.
- Limit foods high in phytates (otherwise known as phytic acid). See above.
- Keep offering great sources of zinc at meals. See below.
Zinc Sources: (extensive list here)
- Oysters (1 oz) – 8 mg
- Beef (4 oz) — 4.09 mg
- Spinach (1 cup) – 1.4 mg
- Eggs (1 medium) — 1 mg
- Lentils (1/2 cup) — 1.25 mg
- Oats (1/4 cup) — 1.55 mg
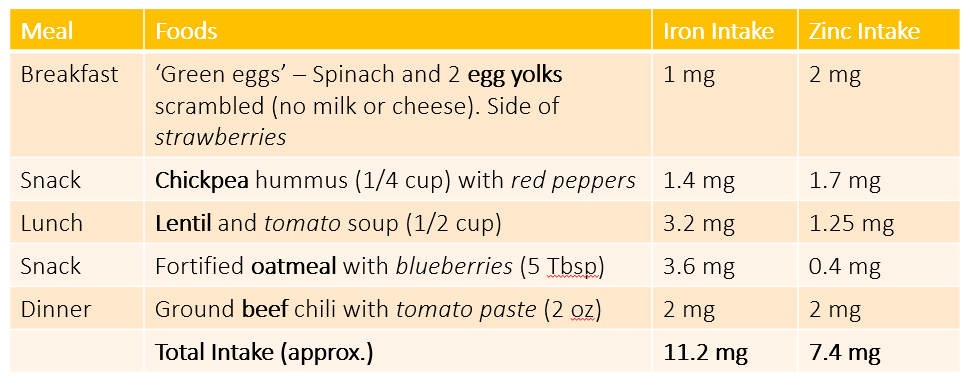
If you’re wondering what a sample meal would look like for your toddler, see below. You’ll notice that there are similar food sources of iron and zinc, so you can kill two birds with one stone! Note: italicized foods are high in vitamin C for better iron absorption.
4) Limit the liquids
Our Sienna LOVED her ‘milk’.
While I loved it too, because it’s a homemade hemp formula chalk full of nutrients, I don’t want it to be her only source of nutrition.
If Sienna had the choice, she would have her ‘milk’ at every meal.
And it would BE her meal.
Eventually, we had to reign it in and restrict milk times to optimize her eating. With consistency and some hardball by mom and dad, Sienna learned that she got milk 3 times a day (upon waking, before nap, and before bed) and that alone improved her appetite.
What’s the message from my little rant?
Limit the liquids.
As mentioned in point #1, no food or drink (except water) should be permitted between meals/snacks. During those meals/snacks, nutrient-dense liquids (i.e. smoothies) and water are OK depending on the child. And, limit the juice. I’d go so far to say avoid juice if you can, especially with selective eaters. The sweetness will be satiating and subdue their appetite, without any of the benefits.
There you have it! These are the main reasons your little one seems to be able to run off fumes most days. But don’t panic!
They are likely taking in exactly how much they need.
That is, as long as we don’t interfere with their innate hunger cues.
Still concerned, let’s chat mom-to-mom.







Fantastic post with great suggestions Danielle! Will definitely try to incorporate some to see if Eddie’s appetite improves!
Glad you found it helpful Viv! Keep me posted on how things go.
Thanks for this great post, the tips are super helpful as are the suggested daily requirements and paired food lists. Seeing this makes me realize my Bean probably isn’t getting enough iron these days.
I guess grandma’s insistence on Bean eating chicken liver wasn’t so far off!
Oh good. There’s no shortage of articles out there pushing the importance of iron (and zinc to a lesser degree), but not many provide tangible ideas for how to achieve the daily recommended dose. That was my goal for this one, so happy to hear you got some goodness out of it:)
And yes, liver is gold and grandma was right!
Wow….this one is really informative. I will reduce milk intake and use Zink supplement. God bless you